News
How is coronavirus disease treated in hospital?
Oxygen therapy
Infected and damaged lungs are less effective at allowing oxygen to pass from the environment to the bloodstream. The main reason for being admitted to hospital with COVID-19 is to receive supplemental oxygen, to increase the amount of oxygen in the lungs and blood, which will be sufficient treatment before recovery in most cases. This can be administered in a number of ways, including into the nose using plastic tubing, or via a loose-fitting face mask.
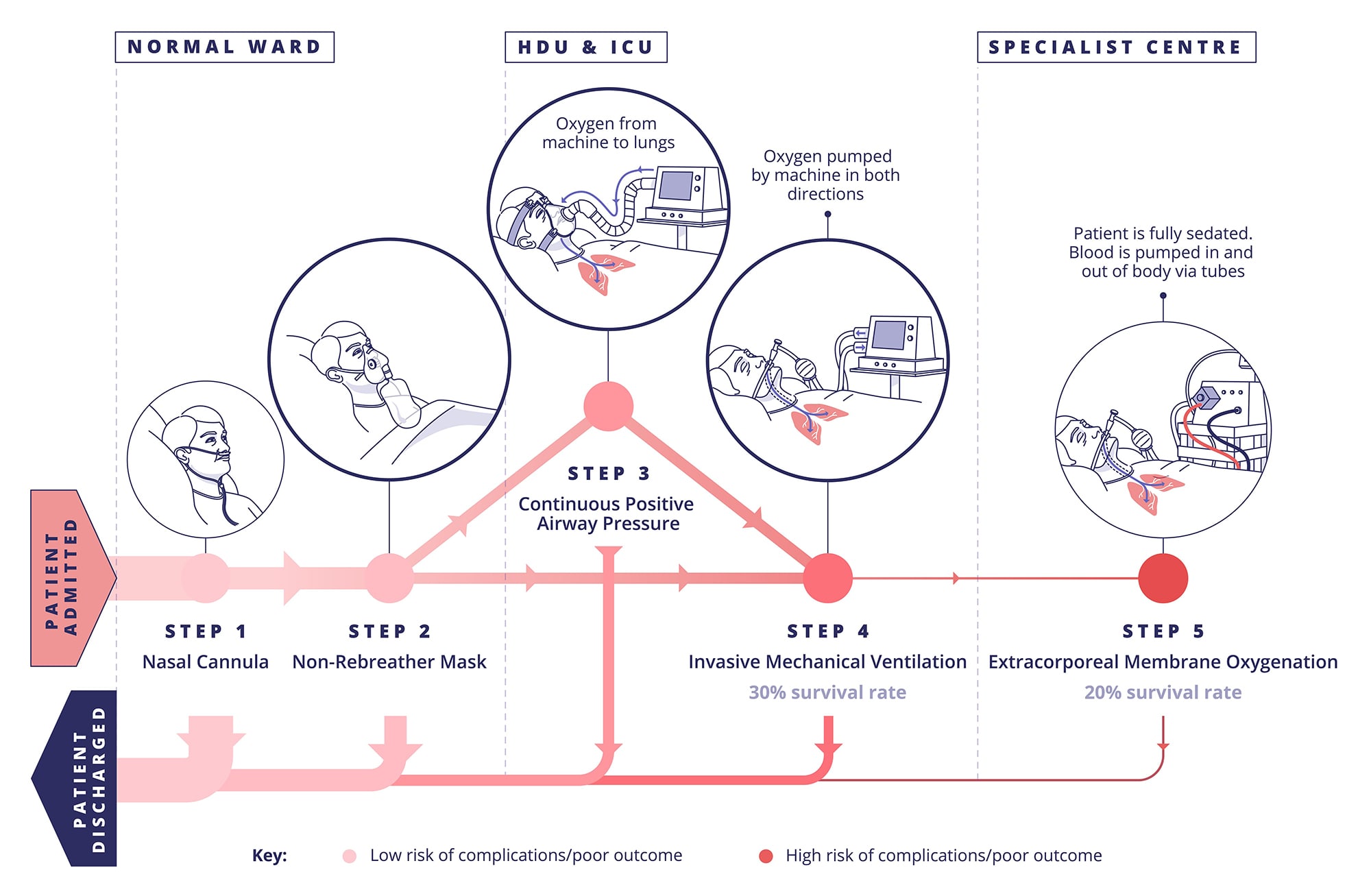
https://coronavirusexplained.ukri.org/en/article/vdt0008/
These patients don’t struggle to breathe—but COVID-19 is still starving them of oxygen
One alarming symptom robs many patients of blood oxygen well before they notice. Doctors are racing to understand it. 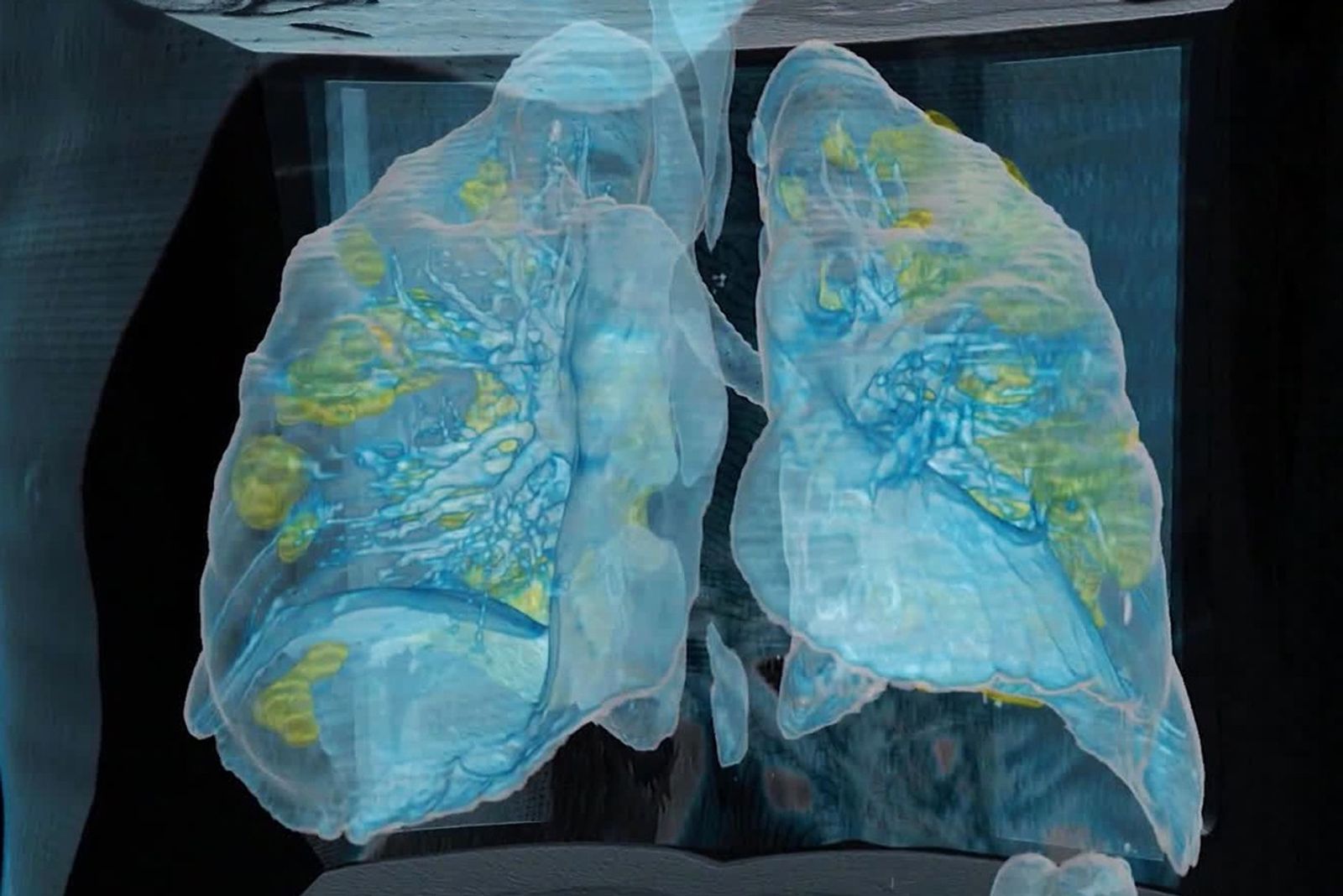
Standing in her patient’s living room, Mari Seim was perplexed. The man, in his 60s, had fallen ill with flu-like symptoms more than a week before. His breathing rate had climbed, so his daughter called the Taarnaasen Medical Centre, the clinic where Seim works as a general practitioner, just outside Oslo, Norway. With COVID-19 at the forefront of her mind, Seim set out to check on the man, and she wasn’t prepared for what she found.
“He was sitting in a chair, and he was smiling,” she says. “He didn’t seem bothered in any way.”
Yet his breaths came in rapid succession, nearly triple the normal rate. A faint blue tinted his lips and fingers. She truly didn’t grasp how sick he was until she measured the oxygen levels in his blood. A normal percentage would sit well above 90. The number Seim saw was 66. For a split second, Seim thought she had the device turned upside down. She checked again. The reading was the same, and she immediately called an ambulance.
Should you be checking your own oxygen levels if you have coronavirus symptoms?
 Oxygen saturation levels are a measure of how much oxygen is getting round your body and can be fairly reliably assessed with a little gadget called a pulse oximeter that clips on to your finger. Two wavelengths of lights are emitted by an LED inside the device on one side of the finger. The light that passes through the fingertip is measured and the amount that has been absorbed by the oxygen in the blood is calculated to give an oxygen saturation – or “sats” – reading. A figure is displayed, which is the percentage of the maximum amount of oxygen that the blood should carry, and the ingenious little gadget – which runs on one AAA battery – also displays heart rate.
Oxygen saturation levels are a measure of how much oxygen is getting round your body and can be fairly reliably assessed with a little gadget called a pulse oximeter that clips on to your finger. Two wavelengths of lights are emitted by an LED inside the device on one side of the finger. The light that passes through the fingertip is measured and the amount that has been absorbed by the oxygen in the blood is calculated to give an oxygen saturation – or “sats” – reading. A figure is displayed, which is the percentage of the maximum amount of oxygen that the blood should carry, and the ingenious little gadget – which runs on one AAA battery – also displays heart rate.
Pulse oximetry is a useful adjunct in deciding who needs treatment, admission to hospital, oxygen therapy, a transfer to intensive care, ventilation and then, at the other end of the tunnel, who can be safely discharged home and reassured that they’re on the mend. Oximeters don’t work well if your hands are cold, you have shellac on your nails or the battery is flat.
What Coronavirus (COVID-19) does to the body.
During this global pandemic, there has been 24 million cases of COVID-19 worldwide. For most the virus is mild, but for some it is fatal, and although governments are trying to contain it, the virus continues to spread. Coronavirus (officially called Sars-CoV-2) will attack your body when somebody coughs nearby and you breath in or if you touch your face after touching a contaminated surface.
Most people will experience the disease as mild. 8 out of 10 people who get coronavirus will have a fever and a cough, some will also get body aches, headaches, and a sore throat. The fever and the feeling of being under the weather is because your immune system is recognising that the virus in invading and therefore is fighting the infection. Due to the irritation of cells, a coronavirus sufferer will have a dry cough, some people may start to cough up a thick mucus called sputum which contains dead lung cells which were killed by the virus. Paracetamol, bed rest and plenty of fluids are the best way to treat these symptoms and you will not need any specialist hospital care.
The percentage of cases of people becoming critically ill from COVID-19 is estimated around 6% and at this stage, the body starts to fail and there is be a chance of death. Organs start to fail and blood pressure drops as the immune system becomes out of control. The lungs become inflamed and stops the body getting the oxygen needed to stay alive. At this point, treatment is crucial and could include ECMO (extra-corporeal membrane oxygenation). But eventually the damage can reach fatal levels at which organs can no longer keep the body alive.







